Respiratory Infections:
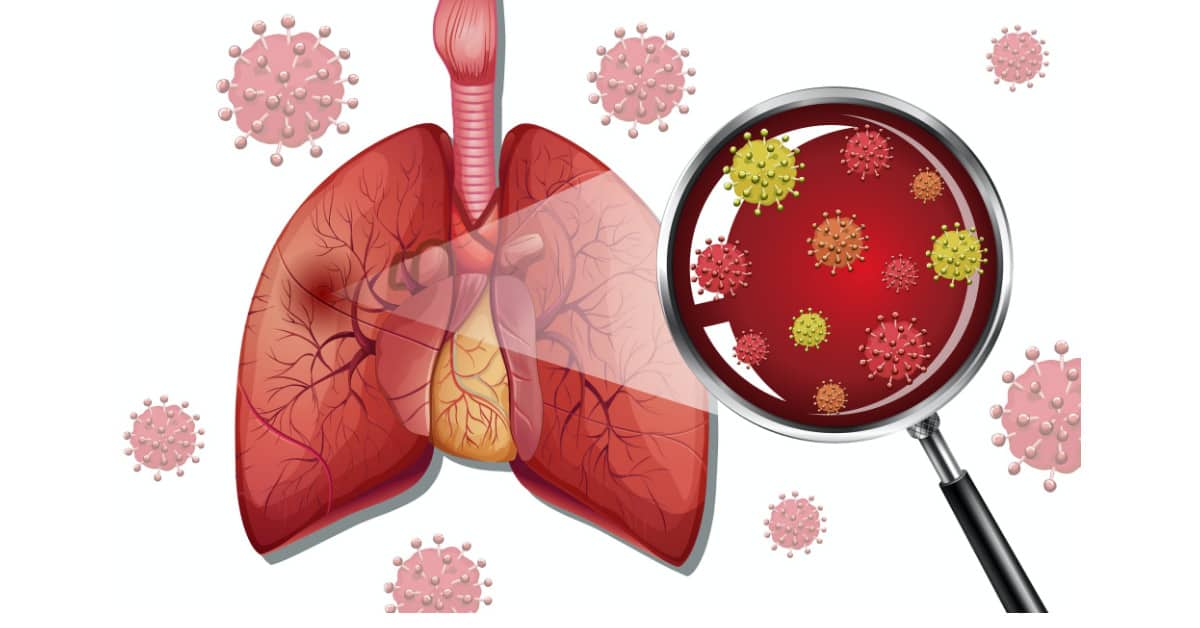
Lungs are an integral part of the respiratory system. There are two lungs in the human body on either side of the heart. They are made up of airways or bronchioles that conduct the air to alveoli or air sacs, which provide area for exchange of gases, oxygen and carbon dioxide.
Infection of the lungs is called pneumonia. It can involve a part of the lung or extend to involve one or both lungs. In pneumonia, the air sacs fill up with infected fluid or pus. The severity of infection depends upon the age and general health condition of the patient, and the type of organism causing the infection. Most commonly, a worsened upper respiratory tract infection may lead to development of pneumonia.
(Read more about respiratory system and infections).
Causes:
Three types of organisms are responsible for causing pneumonia; virus, bacteria, or fungal.
Viral pneumonia is often mild but can worsen in immune-compromised individuals. These are spread rapidly and cause infections in many people at the same time, such as the respiratory syncytial virus (flu virus), SARS-CoV-2 (COVID-19 virus).
Bacteria are the most common organisms involved in pneumonia. It may begin spontaneously but frequently develops secondary to a viral infection, like after flu or a cold. These include Streptococcus pneumoniae, Legionella, Mycoplasma, Haemophilus influenza species. These are also contagious but lesser then viruses.
Fungal pneumonia is rare and affects people with severely compromised immunity, as in cancer or transplant patients. Pneumocystis pneumoniae, Coccidioidomycosis, Histoplasmosis, and Cryptococcus are the usually identified fungal organisms.
Risk factors:
Though pneumonia may occur in any person but certain factors put the patient at more risk. These are:
- Age-younger than 2 years and older than 60 are more at risk
- Recent respiratory infection-flu or cold, cough.
- Having prior lung disease or any chronic disease; diabetes, stroke
- Immune-compromised-cancer patients, on chemotherapy and radiotherapy, transplant patients on immune suppressants, or anyone on immune modulators
- Admitted in ICU for any reason, and on ventilator increases the risk
- Exposure to chemicals, toxic fumes and pollutants
- Malnourished, smoker, alcohol abuse.
Symptoms:
Milder symptoms include cough with phlegm, and fever. Severe cases can present with shortness of breath, chest pains, fever with chills, nausea, vomiting and even diarrhea.
Elderly do not always present with the classical picture of pneumonia, cough and fever. They may present with a chronic cough, mild fever, and mental confusion.
Diagnosis:
A clinical history and proper examination of the chest is a good enough guide for the physician to diagnose pneumonia. Tests are done to confirm the diagnosis, assess the severity, and see the progress of the disease. These are the chest X-ray, full blood count, pulse oximetry, and blood and sputum cultures. In severe cases, the doctor may also advice CT scan of the chest, pleural fluid analysis and culture, and bronchoscopy to look inside airways and collect deep phlegm samples.
Treatment:
Treatment depends upon the type and severity of infection. Viral pneumonias are treated with supportive interventions and occasionally need anti-viral medications. Bacterial pneumonias require antibiotics either orally or intravenous depending on the severity of disease. And anti-fungal treatment is given in fungal pneumonia.
Oxygen therapy, steam inhalation, fever control, and resting constitute the supportive interventions. Ideally, the patient starts improving after 24-48 of antibiotics.
A few score systems have been developed to assess the severity of disease, such as the CURB-65 score and the Pneumonia severity index (PSI). The evaluated factors in these scores include age, gender, blood pressure, pulse, breathing rate, kidney function, mental well being, chronic diseases, and oxygen quantity in the blood.
Complications:
Pneumonia may worsen to form pus collections or abscesses in the lungs. These require long-term antibiotics and surgical drainage. It may extend to involve the lung coverings (pleura) or access to the blood stream leading to full blown infection called sepsis. Sepsis and pneumonia are life-threatening conditions and may lead respiratory and kidney failures.
Prevention:
Upholding of a good hygiene, and leading a healthy lifestyle with frequent exposure to fresh air retains the wellbeing of lungs. In addition, protect yourselves from toxin fumes and chemical including smoking. Avoid crowded places and visiting patients. Regular chest physiotherapy is recommended for people with chronic lung diseases.
Viral pneumonia is prevented by the use of flu vaccines and COVID-19 vaccine.
Some Specific types of Pneumonias:
Community-acquired pneumonia (CAP):
This is the term used when the patient develops pneumonia outside of the hospital or other health care facilities. CAP is the common form of pneumonia and can be secondary to any of three infective organisms.
Hospital-acquired pneumonia (HAP):
HAP is seen in patients who are admitted in hospital for any reason or those who have been discharged in the last 6 weeks. These are usually caused by resistant bacteria that require extensive antibiotics.
Healthcare-acquired Pneumonia (HCAP):
These affect the people in long-term facility centers, or those who frequently visit dialysis units, outpatient departments. HCAP can be viral or secondary to resistant bacteria.
Aspiration Pneumonia:
When a person inhales food or vomit, it irritates the airways and air sacs, resulting in pneumonia. This occurs in stroke patients who have lost their ability to swallow.
Conclusion
Pneumonia is a common treatable lung infection. A timely diagnosis, early initiation of treatment and abiding by the advised protocol prevents worsening of disease and complications. If at any time the patient feels uneasy or shortness of breath, contact the doctor or emergency services.
See Also